Ultrasound-Guided Breast Biopsy: CPT Coding and Comprehensive Overview (Updated 04/09/2026)
This detailed guide navigates the complexities of CPT coding for ultrasound-guided breast biopsies, focusing on accurate billing and reimbursement within the evolving market,
anticipated to reach US $1,090 million by 2032.
Ultrasound-guided breast biopsy has become a cornerstone in the diagnostic evaluation of suspicious breast lesions, offering a minimally invasive approach to tissue acquisition. This procedure utilizes high-frequency sound waves to create real-time images of the breast, allowing physicians to precisely target areas of concern for biopsy. The increasing prevalence of breast cancer and advancements in imaging technology have driven significant growth in this market, projected to reach US $1,090 million by 2032, with an 8% CAGR.
Accurate CPT coding is crucial for appropriate reimbursement and data collection. Understanding the nuances of these codes, particularly 19081, is essential for healthcare providers and billing departments. The global breast biopsy market, encompassing core needle, vacuum-assisted, and fine needle aspiration techniques, is significantly impacted by factors like the COVID-19 pandemic and the strategies of key market players. This overview will delve into the specifics of coding, procedure details, and market trends surrounding ultrasound-guided breast biopsies.
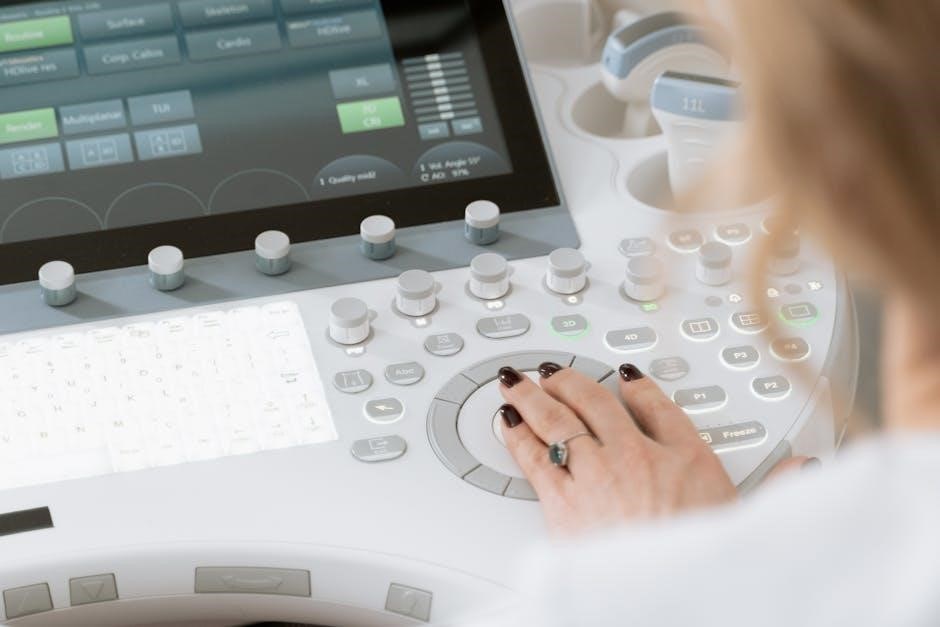
What is an Ultrasound-Guided Breast Biopsy?
An ultrasound-guided breast biopsy is a procedure where a small tissue sample is removed from a suspicious area of the breast using ultrasound imaging for precise guidance. This technique allows for accurate targeting of lesions, minimizing discomfort and improving diagnostic accuracy. It’s a vital component of the growing breast biopsy market, anticipated to reach US $1,090 million by 2032, driven by advancements in imaging and a rising cancer prevalence.
The procedure typically involves using a thin needle, guided by real-time ultrasound images, to collect cells for pathological examination. Proper CPT coding, specifically codes like 19081 and potentially others depending on the technique (core needle vs. vacuum-assisted), is paramount for correct billing. Understanding the market dynamics, including the impact of events like the COVID-19 pandemic and the competitive landscape, is also crucial for healthcare providers navigating this evolving field.
Indications for Ultrasound-Guided Breast Biopsy
Ultrasound-guided breast biopsies are indicated when imaging reveals suspicious findings requiring pathological confirmation. These include newly detected breast lumps, areas of distortion within the breast tissue, or changes following neoadjuvant chemotherapy. The global market for breast biopsies, projected to reach US $1,090 million by 2032, reflects the increasing need for accurate diagnostic procedures.
Specifically, ultrasound is particularly useful for evaluating solid masses and differentiating between benign and malignant lesions. Accurate CPT coding, such as 19081 for the core biopsy, is essential for appropriate reimbursement. The decision to perform a biopsy is often guided by the BIRADS (Breast Imaging Reporting and Data System) assessment category. Understanding the nuances of billing, including potential modifiers, is crucial given the market’s growth and the impact of factors like the COVID-19 pandemic on healthcare access and diagnostic testing.

CPT Codes for Ultrasound-Guided Breast Biopsy
Accurate CPT coding is vital for billing ultrasound-guided breast biopsies, with 19081 being primary; additional codes like 19082 and 77002 may also apply.
Primary CPT Code: 19081
CPT code 19081 represents the core of ultrasound-guided breast biopsy billing. This code specifically covers image-guided percutaneous biopsy of the breast, utilizing ultrasound guidance for precise needle placement. It’s crucial to understand that 19081 encompasses the entire procedure, from ultrasound imaging to the actual tissue acquisition.
However, proper documentation is paramount when utilizing this code. The medical record must clearly demonstrate the use of ultrasound guidance throughout the biopsy process, detailing the imaging findings that led to the targeted biopsy. Furthermore, the report should specify the location and depth of the biopsy, as well as the type of needle used.
It’s important to note that 19081 is a relatively comprehensive code, but it doesn’t automatically include services performed by separate physicians, such as image guidance provided by a radiologist independent of the performing surgeon. In such cases, additional CPT codes may be necessary to accurately reflect the complete scope of services rendered.

19081 ⎻ Detailed Explanation
CPT code 19081, “Image-Guided Percutaneous Biopsy of the Breast,” is the foundational code for billing ultrasound-guided breast biopsies. It includes all related services, from initial ultrasound assessment to the final tissue sample collection. The “image-guided” component is critical; documentation must explicitly confirm real-time ultrasound visualization during the entire procedure.
This code applies to biopsies performed to evaluate suspicious breast lesions identified through imaging. It doesn’t differentiate between lesion size or location within the breast, making it versatile for various clinical scenarios. However, it’s essential to remember that 19081 covers the biopsy itself – not the initial diagnostic imaging that led to the biopsy decision.
Accurate coding requires a clear link between the imaging findings, the biopsy target, and the successful acquisition of a representative tissue sample. The procedure report should detail the technique used (e.g., core needle biopsy, vacuum-assisted biopsy) and any challenges encountered during the process. Proper documentation ensures appropriate reimbursement and avoids potential audit scrutiny.
Additional CPT Codes Potentially Applicable
While 19081 is the primary code, several others may be necessary for complete and accurate billing of an ultrasound-guided breast biopsy. 19082, “Image Guidance for Biopsy (e.g., Real-time Ultrasound, Fluoroscopy, CT Scan),” becomes relevant if a separate physician provides the image guidance services – distinct from the physician performing the actual biopsy. This prevents unbundling and ensures appropriate compensation for each specialist involved.
Furthermore, 77002, “Contrast Agent(s) – Diagnostic, Intraoperative or Image-Guided Procedure(s),” is applicable if a contrast-enhancing agent is utilized during the ultrasound procedure to better visualize the lesion. This is less common in standard breast biopsies but may be employed in specific cases.
Careful consideration of these additional codes is crucial for maximizing reimbursement and adhering to coding guidelines. Documentation must clearly support the use of each code, detailing the services provided and the rationale for their necessity. Failing to appropriately bill for all applicable services can lead to revenue loss.
19082 ⎻ Image Guidance for Biopsy (If Separate Physician)
CPT code 19082 specifically addresses scenarios where a physician separate from the one performing the ultrasound-guided breast biopsy provides the real-time image guidance. This is crucial for accurate billing, preventing the improper unbundling of services. It acknowledges the distinct skill and time involved in precisely navigating the biopsy needle under imaging control.
To appropriately utilize 19082, documentation must clearly demonstrate that a different physician actively guided the biopsy instrument using ultrasound. This isn’t simply overseeing the procedure; it requires real-time direction and adjustments based on the imaging findings.
Without this separation of services, the image guidance component is considered inherent in 19081. Proper application of 19082 ensures both physicians are appropriately compensated for their respective contributions, aligning with payer expectations and avoiding potential audit scrutiny.
77002 ⎻ Contrast Agent (If Used)
CPT code 77002 is reported in conjunction with the primary biopsy code (typically 19081) when a contrast-enhancing agent is administered and utilized during the ultrasound-guided breast biopsy procedure. While not routinely employed, contrast agents can significantly improve visualization of lesions, particularly those with subtle characteristics or located in challenging anatomical areas.
Accurate coding requires meticulous documentation confirming the specific contrast agent used, the dosage administered, and the clinical rationale for its application. Simply stating “contrast used” is insufficient; details are paramount.
Payer policies regarding contrast agent reimbursement vary, so verifying coverage prior to administration is prudent. 77002 represents the cost of the agent itself, separate from the professional component of the biopsy and image guidance. Proper utilization ensures appropriate reimbursement for this potentially valuable adjunct to the diagnostic process.

Procedure Details & Techniques
Ultrasound guidance facilitates precise needle placement for core or vacuum-assisted biopsies, enhancing diagnostic accuracy and minimizing patient discomfort, crucial for correct CPT code application.
Types of Ultrasound-Guided Breast Biopsies
Several techniques fall under the umbrella of ultrasound-guided breast biopsy, each with specific applications and, consequently, potential CPT code implications. Understanding these distinctions is vital for accurate billing;
Core Needle Biopsy
This is a commonly performed procedure utilizing a large-bore needle to extract tissue samples for pathological analysis. It’s often the first-line approach for evaluating suspicious lesions identified on imaging. The primary CPT code, 19081, frequently applies to this technique, though modifiers may be necessary depending on the complexity and number of samples taken. Proper documentation detailing the lesion characteristics and sampling technique is crucial for justifying the code.
Vacuum-Assisted Biopsy (VAB)
VAB employs a vacuum to collect larger tissue samples through a single insertion, potentially reducing the number of needle punctures. While 19081 can sometimes be used, VAB often requires additional coding considerations, particularly if multiple lesions are targeted or if contrast is utilized. The global breast biopsy market anticipates growth, and VAB is a significant contributor to this expansion, necessitating precise coding practices to reflect the procedure’s complexity.
The core needle biopsy represents a foundational technique in ultrasound-guided breast tissue acquisition, frequently coded with 19081. This procedure involves utilizing a large-bore needle, guided by real-time ultrasound imaging, to obtain cylindrical tissue samples from suspicious breast lesions.
Accurate CPT coding hinges on meticulous documentation. Details regarding lesion size, location, depth, and the number of cores extracted are paramount. If multiple lesions are biopsied during a single session, appropriate modifiers should be appended to 19081 to reflect the increased work. The global breast biopsy market, projected to reach US $1,090 million by 2032, sees core needle biopsies as a significant component.
Furthermore, consider if image guidance was provided by a separate physician (potentially requiring 19082) or if contrast agents were employed (potentially requiring 77002). Proper coding ensures appropriate reimbursement and reflects the complexity of the procedure.
Vacuum-Assisted Biopsy (VAB) is a more advanced ultrasound-guided technique, often utilized for larger lesions or when multiple samples are required, and is typically coded utilizing 19081 alongside potential modifiers. VAB employs a vacuum device to collect larger, more representative tissue cores through a single insertion.
CPT coding for VAB requires careful attention to detail. Documentation should clearly indicate the number of vacuum passes performed and the total volume of tissue removed. As the global breast biopsy market anticipates reaching US $1,090 million by 2032, VAB’s efficiency contributes to market growth.
Similar to core needle biopsies, consider additional codes like 19082 if image guidance is provided by a separate physician, or 77002 if contrast agents are utilized. Accurate coding is crucial for maximizing reimbursement and reflecting the increased complexity and resource utilization associated with VAB procedures.
The Biopsy Procedure: A Step-by-Step Guide
The ultrasound-guided breast biopsy procedure begins with patient positioning and skin preparation, followed by real-time ultrasound visualization to identify the target lesion. Local anesthesia is administered to minimize discomfort during the biopsy.
A sterile needle, guided by the ultrasound, is then inserted into the lesion to obtain tissue samples. For core needle biopsies, multiple passes may be needed, coded primarily with 19081. Vacuum-assisted biopsies (VAB) utilize a different device, also generally coded with 19081, but potentially requiring more detailed documentation.
Post-biopsy, pressure is applied to the site to control bleeding, and a compression bandage is applied. Proper documentation, including the CPT code(s) used, is vital for accurate billing, especially considering the projected US $1,090 million market size by 2032. Accurate coding ensures appropriate reimbursement for these essential diagnostic procedures.
Patient Preparation and Post-Biopsy Care
Prior to an ultrasound-guided breast biopsy, patients are typically advised to discontinue blood-thinning medications as directed by their physician. They should also inform their doctor of any allergies or medical conditions.
During the procedure, patients remain still while the ultrasound guidance ensures accurate tissue sampling, often coded as 19081. Post-biopsy, patients receive instructions on wound care, including keeping the area clean and dry. Mild discomfort or bruising is common.
Follow-up appointments are scheduled to discuss biopsy results. Accurate CPT coding, crucial in a market projected to reach US $1,090 million by 2032, impacts reimbursement. Patients should report any signs of infection, such as fever or increased pain, promptly. Proper care optimizes healing and accurate diagnosis.

Market Trends and Future Outlook
The global ultrasound-guided breast biopsy market is experiencing substantial growth, projected to reach US $1,090 million by 2032, driven by advancements and accurate CPT coding.
Global Breast Biopsy Market Size & Growth (2022-2032)
The global breast biopsy market, encompassing core needle, vacuum-assisted, and fine needle aspiration techniques, is currently experiencing a period of significant expansion. Recent analysis indicates a substantial market size with promising growth projections extending through 2032. Specifically, the Ultrasound-Guided Breast Biopsy segment is anticipated to achieve sales of US $1,090 million by 2032.
This impressive growth is fueled by a Compound Annual Growth Rate (CAGR) of 8% during the forecast period (2022-2032). Several factors contribute to this positive trajectory, including increasing breast cancer incidence rates globally, advancements in imaging technologies – particularly ultrasound guidance – and a growing emphasis on early detection and minimally invasive diagnostic procedures. Accurate CPT coding practices are crucial for maximizing reimbursement and supporting continued market investment.
The market’s evolution is also influenced by the ongoing impact of the COVID-19 pandemic, which initially disrupted diagnostic services but has subsequently spurred innovation in remote monitoring and streamlined biopsy workflows. Understanding these market dynamics is essential for healthcare providers and industry stakeholders alike.
Impact of COVID-19 on the Market
The COVID-19 pandemic initially presented significant challenges to the ultrasound-guided breast biopsy market, causing disruptions in routine screening programs and elective procedures. Healthcare facilities faced capacity constraints and prioritized emergency care, leading to delays in diagnostic evaluations. This temporary decline underscored the importance of adaptable billing practices and accurate CPT coding to maintain revenue streams during periods of reduced volume.
However, the pandemic also catalyzed innovation within the market. The need for reduced patient contact and streamlined workflows spurred the adoption of remote monitoring technologies and enhanced safety protocols. Furthermore, the backlog of delayed screenings is now driving increased demand for biopsies, potentially leading to a surge in procedure volumes.
Consequently, a renewed focus on efficiency and optimized resource allocation is crucial. Accurate CPT coding, coupled with a thorough understanding of evolving payer policies, will be paramount for maximizing reimbursement and navigating the post-pandemic landscape.
Key Players in the Ultrasound-Guided Breast Biopsy Market
Several prominent companies are shaping the ultrasound-guided breast biopsy market, each contributing to advancements in technology and procedural techniques. These key players are actively involved in developing and distributing core needle biopsy systems, vacuum-assisted biopsy (VAB) devices, and associated imaging solutions. Accurate CPT coding is essential for these companies to demonstrate the value of their offerings and secure appropriate reimbursement.
Understanding the competitive landscape requires monitoring their strategies regarding product innovation, market penetration, and partnerships. These companies often provide resources and training to healthcare providers on proper procedure coding and billing practices.
Furthermore, their influence extends to shaping industry standards and advocating for favorable payer policies. Maintaining a current understanding of their product portfolios and coding recommendations is vital for optimizing revenue cycle management and ensuring compliance within the evolving market.
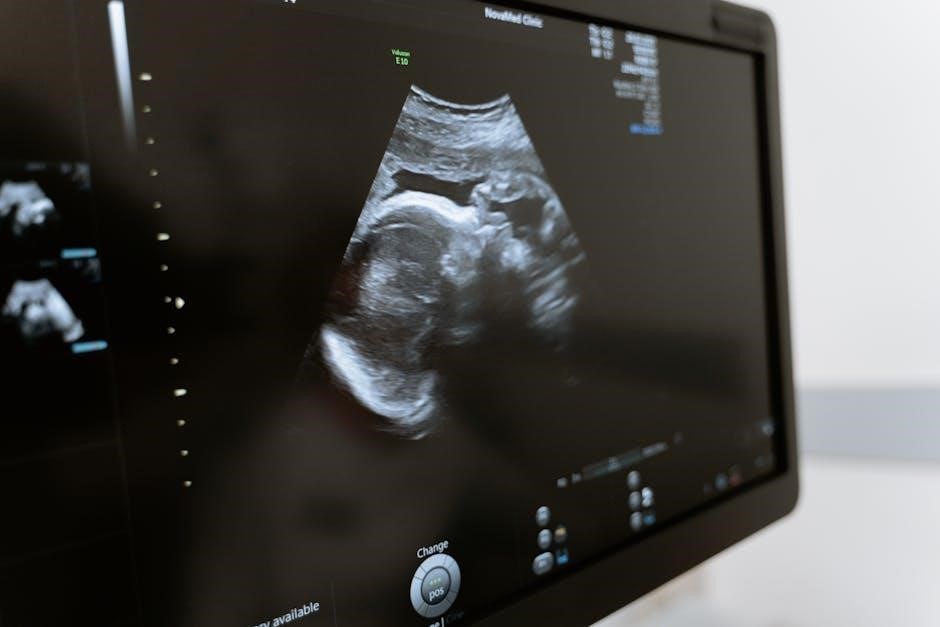
Billing and Reimbursement Considerations
Navigating billing requires precise CPT code application, alongside modifier usage, to reflect services accurately. Payer policies significantly impact reimbursement rates for ultrasound-guided breast biopsies.
Coding Modifiers for Ultrasound-Guided Biopsies
Accurate modifier application is crucial for appropriate reimbursement when billing for ultrasound-guided breast biopsies. Modifiers provide additional information to payers regarding specific circumstances of the procedure. For instance, modifier -RT (Right side) or -LT (Left side) must be appended to the primary CPT code (19081) to indicate the breast biopsied.
Modifier -59 (Distinct Procedural Service) is frequently utilized when multiple biopsies are performed on the same breast during a single session, ensuring each biopsy is billed separately. If the biopsy is performed under the direction of a different physician than the one providing the ultrasound guidance, modifier -FS (Facility Service) or -GC (Image Guidance) may be necessary, potentially linking to code 19082.
Carefully review payer-specific guidelines as modifier usage can vary. Incorrect modifier application or omission can lead to claim denials or reduced reimbursement. Staying updated on coding changes and payer policies is essential for maximizing revenue and ensuring compliance within the evolving ultrasound-guided breast biopsy market.
Common Billing Errors to Avoid

Several common billing errors can lead to claim denials when submitting charges for ultrasound-guided breast biopsies. A frequent mistake is incorrect CPT code selection; ensure 19081 accurately reflects the procedure performed. Failing to append laterality modifiers (-RT or -LT) is another common error, resulting in incomplete claims.
Improper use of modifier -59 when billing for multiple biopsies during a single session is also prevalent. Payers often scrutinize claims with this modifier, requiring clear documentation justifying each separate procedure. Incorrectly billing for contrast agent (77002) when it wasn’t utilized, or omitting it when it was, is a significant error.
Insufficient documentation supporting the medical necessity of the biopsy is a frequent cause for denial. Finally, lack of awareness of payer-specific policies regarding coding and coverage can lead to consistent claim rejections. Thorough coding audits and staff training are vital for minimizing these errors and optimizing revenue cycle performance within the growing US $1,090 million market.
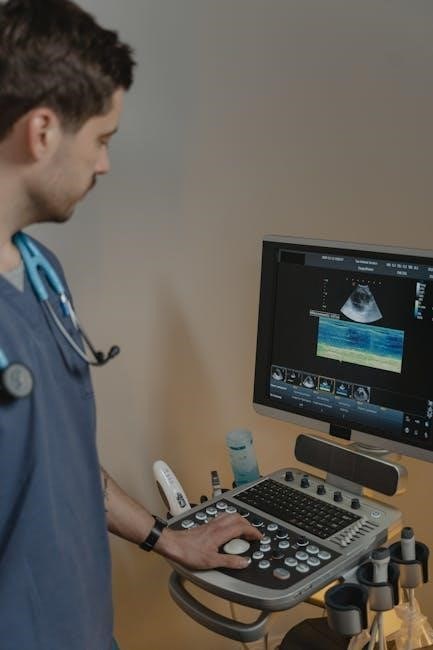
Reimbursement Rates and Payer Policies
Reimbursement rates for ultrasound-guided breast biopsies (CPT 19081) vary significantly based on payer type, geographic location, and negotiated contracts. Medicare generally establishes a benchmark rate, which commercial insurers often follow, though with variations. Expect regional differences impacting final reimbursement amounts.
Payer policies often dictate specific documentation requirements, including imaging reports, pathology results, and clinical indications supporting medical necessity. Pre-authorization may be required by some insurers, particularly for vacuum-assisted biopsies (VAB). Understanding these policies is crucial for clean claim submission.
Denials are common due to coding errors or lack of supporting documentation. The global market, projected to reach US $1,090 million by 2032, demands diligent attention to payer guidelines. Staying updated on policy changes and appealing denied claims effectively are essential for maximizing revenue and navigating the complex reimbursement landscape.